Coughs and sneezes, and runny noses are a part of life for every parent of a toddler. Studies suggest that the average child under the age of two has approximately 12 upper respiratory infections per year. That’s right, that works out to about one a month! That’s normal!

Coughs and sneezes: what works- and what doesn’t?
Although its reassuring to know having an almost permanently sick child is normal, its still hard work. Dealing with coughs and sneezes, runny noses, fevers and general crankiness (on top of the usual toddler crankiness) can get a bit wearing. Knowing that your child is developing a healthy immune system with all this exposure to viruses is only a little bit comforting when you’re sleep deprived and exhausted!
The Common Cold:
Coughs and sneezes are often referred to as “the common cold”. In fact, there are literally hundreds of viruses that can cause coughing and sneezing in young children… so it really is very common.
Viruses that affect the upper respiratory tract, such as influenza and rhinovirus, cause inflammation of the lining of the respiratory tract. The respiratory tract includes the nose and mouth, and the throat all the way down to the lungs (the lower respiratory tract). The ears are attached to the nose and soft palate, and are often involved in upper respiratory tract infections.
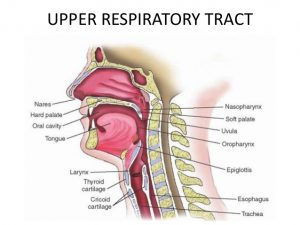
Anatomy of the Upper Respiratory Tract
The inflammation triggers excess mucous production leading to runny nose and congestion. Coughing is caused both by irritation and inflammation of the lining of the respiratory tract, and the excess mucous production. Your child may complain of pain in the throat or itchy nose and eyes.
Coughs and Sneezes: When To Worry
The vast majority of coughs and colds are benign and self- limiting. Even if you do absolutely nothing at all, they generally last around 7 to 10 days and get better by themselves. Most toddlers will be a bit snotty and grumpy, and even more off their food than usual for a few days then gradually sort themselves out.
However, there are some signs you should not ignore. These are what I call “red flag” symptoms, that should prompt you to see a doctor:
- Laboured breathing: you can observe this by looking at your child’s chest. Is he breathing more rapidly than usual? Can you see his rib cage drawing in with each breath? Can you see his windpipe (trachea) “sucking in” at the top of the breastbone? Does he seem to be breathless, or unable to speak as well as normal? These are signs your child needs immediate medical attention.
- Lethargy: all of us feel a little tired when we have the “flu”. If your child wants to sit on the sofa watching endless repeats of their favourite Disney movie, this is fine. However, a listless and excessively sleepy child is cause for concern.
- Poor feeding: although it is usual for children to refuse their solids when they are feeling congested and sick, it is important that you keep them well hydrated. Nothing terrible will happen if they don’t take much food for a couple of days. Conversely, a child can become very unwell if they are allowed to become dehydrated.
- Prolonged high fever: a temperature of greater than 38 degrees centigrade (100.4 fahrenheit) is regarded as fever. If you have a newborn baby (less than 30 days old) with fever, you should seek medical attention urgently. A baby under three months with fever should be seen as soon as possible by a doctor. If you have an older child with fever and none of the other “red flag” symptoms, then you can monitor him at home for a couple of days. You should seek medical attention if it doesn’t seem to be improving after 2-3 days.
Treatment of Coughs and Sneezes:
Home Remedies and Non- Pharmaceutical Treatments:
What Works:
- Saline Spray: you can try squirting a nasal saline spray up your child’s nostrils to relieve nasal congestion and irritation. The physiological saline will help to decongest the nose and relieve itchiness.
- Honey: (Caution- do not give to babies under 12 months of age due to risk of botulism infection). Several studies have pitted the soothing and cough- relieving effects of honey against common over the counter cough remedies- and guess which one came out on top? That’s right- honey consistently outperforms most cough syrups on the market! Simply dissolve a teaspoon of honey in some warm water, add a squeeze of lemon if you like, and allow your child to sip it as required.
- Vitamin C: Vitamin C and zinc are major components of a healthy immune system. Vitamin C can be found in fruits such as grapes, kiwis and blueberries. If your child flat-out refuses to take any vitamin C containing fruits, you may consider a short course of vitamin C supplementation.
- Vicks Baby Balsalm: good old Vicks Vaporub (use the kiddie version, not the adult version if you don’t want your child to complain of stinging!) apparently does work. A study done comparing Vicks to placebo showed reduced coughing duration and severity. You can only use it on children over three months of age, though.
- Tilt the head of your child’s cot or bed slightly so that they are not lying totally flat. Roll a blanket and place it under the mattress of the cot, or pop a few books under the legs of the cot for a small child. Never place pillows in the cot of a small child where they may pose a risk of suffocation.
The Jury Is Out On:
- Chopped onions at the foot of the bed
- Vicks applied on the feet (!)
Over The Counter Remedies and Pharmaceutical Interventions:
- Antihistamines: antihistamines act by reducing histamine release; as histamine is responsible for inflammation and subsequent mucous production, reducing histamine release seems like a good strategy. Unfortunately, antihistamines have consistently failed to demonstrate significant improvement in scientific studies. Some antihistamines such as promethazine are prescribed as cough suppressants- avoid giving these to young children, as they may suppress respiratory drive.
- Decongestants: these include oxymetazoline-containing medications such as “Iliadin” and “Dimetapp”. These may be useful for short term relief of congestion. They should not be used for more than five consecutive days, unless on the specific advice of your doctor, due to concerns about dependency and rebound nasal congestion after stopping the drug.
- Mucolytics: designed to break down phlegm and make it easier to remove. These drugs have shown themselves to be phenomenally valuable in the treatment of chronic conditions such as cystic fibrosis. Doctors in many countries use drugs such as “Fluimucil” to break down phlegm in the treatment of viral respiratory infections with good effect. Do not use this medication in very young infants unless your doctor has specifically instructed you to- the increase in secretions can sometimes be hazardous to small babies.
- Antibiotics: the majority of coughs and sneezes are caused by viruses, and not bacteria. Antibiotics are designed to treat bacterial infections and not viral infections. Historically, antibiotics have been excessively over-prescribed in the treatment of viral respiratory infections- they will not help to treat your child if he has a viral infection. Antibiotics are occasionally indicated for treatment of a severe bacterial infection or prolonged respiratory infection lasting more than three weeks.
What have you found works for your child? Join the conversation by adding your comment below.
If you have enjoyed reading this article, don’t forget to subscribe to receive weekly medical and parenting advice direct to your inbox. Have a great week ahead.

Leave A Reply