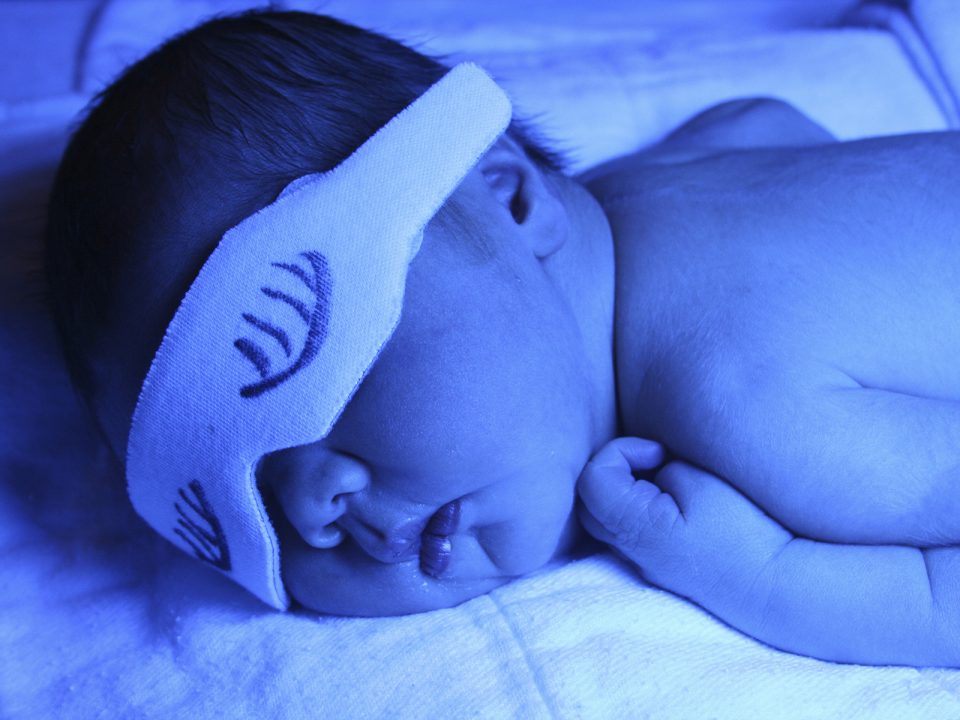
Newborn Jaundice: What’s It All About?
October 1, 2017
Jaundice- the yellowish discolouration of the skin that occurs in around 50% of full term well babies (and up to 80% of babies born prematurely). Most of us will have seen it at some point, but what is it, and […]
No Comment