So your child is driving you crazy with his constant scratching of his skin, and the dreadful red marks he leaves all over his body. When you ask him to stop, he says he can’t- it’s too itchy! What can you do to help him?
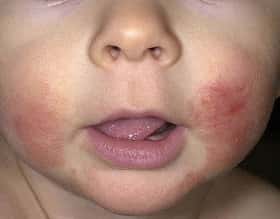
Childhood eczema: image courtesy of National Eczema Society
What Is Childhood Eczema?
Childhood eczema, or atopic dermatitis, is a dry and irritated skin condition caused by sensitivity to various factors. Infants with eczema often have red scaly skin over their cheeks. Older children have redness and flaking of the skin in the skin creases, or joint flexures, such as elbows and backs of knees.
Over time, excessive inflammation of the skin may cause skin thickening (called lichenification) and plaque formation over the affected parts of the body.
Eczema is a relapsing and remitting condition. Unlike other diseases, we cannot treat it and make it go away. There will be times in your child’s life when the condition is better, and when it is worse. It is important to learn what triggers exacerbate your child’s eczema, and how best to manage it.
How common is Childhood Eczema?
Childhood and infantile eczema is common. Around 10% of children under the age of 12 months will have some degree of itchy dry skin; fortunately many grow out of the tendency by later childhood. Some children go on to have chronically dry irritated skin for many years.
Risk factors include:
- Parents or first degree relatives with eczema or environmental allergies.
- HIstory of other “allergic” conditions, such as asthma, allergic rhinitis or seasonal allergies.
What Makes Childhood Eczema Worse?

Sand can irritate dry and sensitive skin
- Environmental conditions; some children find that their eczema becomes worse in dry winter conditions; others have flare ups in hot humid weather, when they are more sweaty.
- Exposure to harsh chemicals: the chlorine in swimming pools can often exacerbate sensitive, dry skin conditions.
- Emotional stress: fear and anxiety can lead to release of hormones that may worsen eczema.
- Adolescent hormonal surges: some children find that their eczema worsens during adolescence.
I’m often asked whether food allergies and sensitivities are linked to childhood eczema. The answer is “no” in the vast majority of cases. Large studies of children with eczema have failed to show any causative food allergy, despite what many parents believe.
It can also be dangerous to cut out various different foods in the belief that they are causing your child’s eczema: your child may be deprived of important nutrients, and may even develop severe vitamin and mineral deficiencies as a result.
What Makes Childhood Eczema Better?
- Reduce exposure to known triggers: of course, you can’t ask your child to stop swimming, but you can make sure that he washes himself immediately rather than running around covered in chlorine for several hours afterwards.
- Stop using soap- based cleansers: soap dries the skin. Instead, choose non-soap cleansers such as QV, Cetaphil, Sebamed, etc.
- Reduce baths in favour of showers: baths are more drying to the skin that showers (bubble-baths are the worst, I’m afraid- you will have to find some other treat for a little girl with eczema). If you absolutely must use a bath (and this is often preferable with small babies) add half a capful of an emulsifying oil such as Oliatum or QV Oil into the bath water.
- Although biological washing detergents are undoubtedly better for the environment, many children with sensitive skin react to the enzymes. Consider changing to a non-biological washing detergent; some children with very sensitive skin may benefit from you washing their clothes in an extra rinse cycle.
- Dress your child in light cotton clothes: these allow the skin to breathe and reduce sweating. Cotton also reduces skin irritation compared to polyester and other man made fabrics. Wool clothing is also more likely to cause excessive itching.
Medical Therapies:
Moisturisers:
Also known as emollients: these are the mainstay of eczema treatment. In dry conditions, emollients used are often thick and oil based, such as paraffin. In hot and humid climates, emollients are water based lotions to reduce the risk of additional sweating and itchiness.
In both dry and humid climates, keeping the skin well moisturised is crucial to reducing itch in childhood eczema. Although the media is full of stories of miracle creams for eczema, the truth is less satisfactory. There is no one miracle cream that will work for everyone. The reality is that you will probably have to try a few different creams until you find one that works well for your child.
Aim to moisturise your child’s skin at least twice a day. The best time to moisturise in within 2-3 minutes after a shower, as the skin will more readily absorb the cream then.
Steroids and Immune Modulators:
Steroids occur naturally in our bodies- they help to reduce inflammation and prevent secondary damage. Doctors prescribe steroids to reduce itch and prevent scratching. They act by reducing inflammation and therefore stop the irritation.
Overuse of steroids is associated with thinning of the skin. It is important to only use a small amount, and only on the irritated skin- do not use steroids on normal skin. Do not apply steroids onto broken skin, or on skin you suspect may be infected. Do not use steroids as a moisturiser. You should apply your child’s moisturiser on top of the steroid cream.
Your doctor will prescribe the lowest strength of steroid he or she feels will be able to control the symptoms. It may be necessary to increase the potency of the steroid if you are not getting control of your child’s symptoms. Your doctor will usually try to reduce the potency or the frequency of application of the steroids once the symptoms are under control.
Other medications are sometimes used (such as tacrolimus and pimecrolimus), which also modulate the immune system’s response to inflammation. These medications can have rare but serious side effects; your doctor will discuss these with you before commencing this medication if required.
Complications Of Childhood Eczema:
Let your doctor know if your child’s eczema changes. If you can see little pockets of pus, or it is weepy, or has golden coloured crusts on the surface, he may have a secondary infection.
Common infections occuring in children with eczema include:
- Staphylococcus (Staph): this can usually be treated with topical antibiotic creams. More severe forms or widespread infections may require oral antibiotics.
- Herpes virus (cold sore virus): this may require topical and oral antiviral treatment such as aciclovir.
Please leave your comments in the box below. If you have found this article useful, don’t forget to sign up for weekly emails delivered directly to your inbox. Have a great week ahead!

Leave A Reply